با علائم و روشهای درمان کاردیومیوپاتی یا بیماری ماهیچه قلب آشنا شوید
کاردیومیوپاتی، بیماری ماهیچه قلب
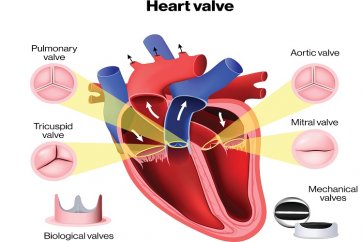
کاردیومیوپاتی انواع مختلفی دارد که در اثر عوامل مختلفی ایجاد میشوند؛ از جمله در اثر بیماری کرونری قلب و داروهای خاص. این عوامل ممکن است باعث بینظمی در ضربان قلب، نارسایی قلبی، بیماری دریچهای قلب و سایر بیماریها شود.
انواع کاردیومیوپاتی
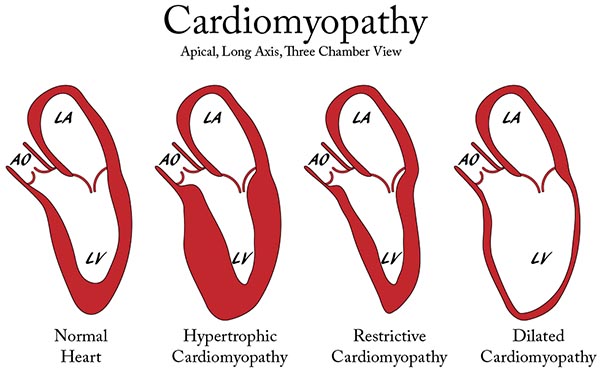
1- کاردیومیوپاتی گشاد شده:
شایعترین نوع کاردیومیوپاتی است. زمانی رخ میدهد که ماهیچه قلب به قدری ضعیف است که نمیتواند خون را به خوبی پمپاژ کند. ماهیچهها دچار کشیدگی شده و نازک میشوند.
این نوع بیماری موجب گشاد شدن اتاقکهای قلب میشود. این نوع کاردیومیوپاتی به «بزرگی قلب یا تورم قلب» نیز شناخته میشوند. ممکن است این بیماری ارثی باشد یا در اثر بیماری عروق کرونری ایجاد شود.
2- کاردیومیوپاتی هایپرتروفیک:
این نوع کاردیومیوپاتی ژنتیکی است. زمانی رخ میدهد که دیوارههای قلب ضخیم شده و مانع از پمپاژ و به گردش درآمدن خون میشود.
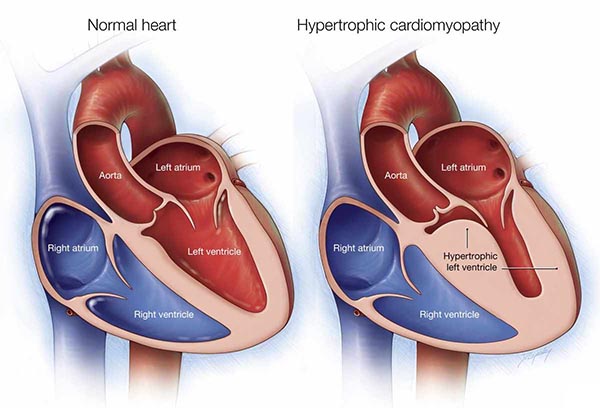
این نوع بیماری، از انواع نسبتا شایع کاردیومیوپاتی است و ممکن است در اثر بالا بودن طولانی مدت فشارخون یا افزایش سن نیز رخ دهد. دیابت یا بیماری تیروئید نیز میتواند این نوع کاردیومیوپاتی را ایجاد کند. عوامل دیگر این نوع بیماری نامشخص است.
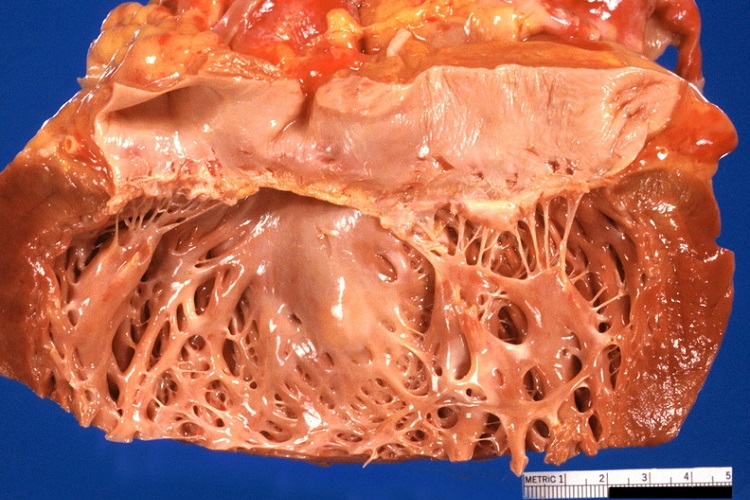
3- دیسپلازی آریتموژنیک بطن راست (ARVD):
این نوع بیماری، از انواع بسیار نادر کاردیومیوپاتی است، ولی عامل اصلی مرگ ناگهانی در ورزشکاران جوان است. در این نوع کاردیومیوپاتی ژنتیکی، بافت چربی یا فیبروز اضافی جایگزین ماهیچه بطن راست میشود که ریتم طبیعی قلب را برهم میزند.
4- کاردیومیوپاتی محدودکننده:
این نوع بیماری، کمترین شیوع را در بین انواع دیگر کاردیومیوپاتی دارد. زمانی رخ میدهد که بطنهای قلب سفت و منقبض شده و نمیتواند برای پر شدن از خون، منبسط شود. اسکار قلب که غالبا به دنبال عمل پیوند قلب ایجاد میشود، میتواند یکی از دلایل این نوع کاردیومیوپاتی باشد. همچنین ممکن است در نتیجه بیماری قلبی نیز رخ دهد.
سایر انواع کاردیومیوپاتی
سایر انواع کاردیومیوپاتی مربوط به یکی از 4 تقسیمبندی فوق است اما هر کدام دلایل خاص خود را دارد:
1- کاردیومیوپاتی بارداری:
در طول بارداری یا پس از آن رخ میدهد. این نوع کاردیومیوپاتی زمانی ایجاد میشود که ظرف 5 ماه بعد از زایمان یا در طول ماه آخر بارداری، قلب ضعیف میشود. وقتی پس از زایمان رخ میدهد، گاها به آن کاردیومیوپاتی پس از زایمان (postpartum) گفته میشود.
این نوع بیماری، یکی از انواع کاردیومیوپاتی گشاد شده است که مرگآور است. دلیل این بیماری نامعلوم است.
2- کاردیومیوپاتی الکلی:
در اثر مصرف بیش از حد الکل در طولانی مدت رخ میدهد که باعث ضعیف شدن قلب میشود لذا قلب دیگر نمیتواند خون را به خوبی پمپاژ کند. سپس قلب بزرگ میشود. این بیماری جزء کاردیومیوپاتی گشاد شده است.
3- کاردیومیوپاتی ایسکمیک:
زمانی رخ میدهد که قلب به خاطر بیماری عروق کرونری، دیگر نمیتواند خون را به اعضای بدن برساند. رگهای خونی عضله قلب باریک و ضخیم میشوند. این موجب نرسیدن اکسیژن به عضله قلب میگردد. کاردیومیوپاتی ایسکمیک از علل شایع نارسایی قلب است.
کاردیومیوپاتی غیر ایسکمیک یکی دیگر از انواع کاردیومیوپاتی است که ارتباطی به بیماری عروق کرونری ندارد. کاردیومیوپاتی غیرفشردگی، که کاردیومیوپاتی اسفنجی نیز نامیده میشود، یکی از بیماریهای نادر مادرزادی است.
این بیماری ناشی از رشد غیرطبیعی عضله قلب جنین در شکم مادر است. در مراحل مختلف حیات جنین امکان تشخیص وجود دارد. زمانی که کاردیومیوپاتی در کودک پدید میآید، به آن کاردیومیوپاتی اطفال (pediatric) گفته میشود.
چه کسانی در معرض خطر کاردیومیوپاتی قرار دارند؟
- سابقه فامیلی کاردیومیوپاتی، ایست قلبی یا نارسایی قلبی
- بیماری عروق کرونری
- دیابت
- چاقی شدید
- سارکوئیدوز
- هموکروماتوز
- آمیلوئیدوز
- سکته قلبی
- فشارخون بالا در طولانی مدت
- اعتیاد به مصرف الکل
علائم کاردیومیوپاتی چیست؟
علائم انواع کاردیومیوپاتی اغلب مشابه یکدیگر است. در تمام انواع این بیماری، قلب نمیتواند خون را به اندازه کافی به بافتها و اندامهای بدن برساند که موجب بروز علائم زیر میشود:
- ضعف و خستگی عمومی
- تنگی نفس، به خصوص در طول ورزش یا کار شدید
- سرگیجه و گیجی و منگی
- درد قفسه سینه
- تپش قلب
- غش کردن
- فشارخون بالا
- اِدِم یا تورم پا، قوزک پا یا ساق پا
آشنایی با روشهای درمان کاردیومیوپاتی
درمان این بیماری بسته به نحوه آسیبدیدگی قلب و علائم آن، متفاوت است. برخی از افراد ممکن است تا بروز زمان علائم، نیازی به درمان نداشته باشند. سایر افرادی که به تازگی دچار تنگی تنفس شدهاند یا درد قفسه سینه دارند، باید سبک زندگی خود را تغییر داده یا دارو مصرف کنند.
امکان درمان کاردیومیوپاتی وجود ندارد، ولی میتوان با رعایت موارد زیر، آن را کنترل کرد:
- تغییر سبک زندگی
- مصرف داروهای درمان فشارخون بالا، جلوگیری از نگهداری آب، حفظ ضربان طبیعی قلب، جلوگیری از ایجاد لختههای خون، کاهش التهاب
- جراحی برای نصب دستگاههایی مثل ضربانساز و الکتروشوک
چهوقت به پزشک مراجعه کنیم؟
زمانی به دکتر مراجعه کنید که یک یا چند نشانه از کاردیومیوپاتی را داشته باشید. برخی از گونهها موروثی هستند. اگر در خانواده شما این بیماری وجود داشته باشد، پزشک تمام اعضای خانواده را معاینه میکند.
روشهای پیشگیری از کاردیومیوپاتی
در بیشتر مواقع، نمیتوان از این بیماری پیشگیری کرد. شما میتوانید با تغییر دادن سبک زندگی خود، تا حد زیادی کاردیومیوپاتی را مهار کنید:
- از مصرف کوکائین و الکل خودداری کنید.
- دخانیات مصرف نکنید.
- فشارخون بالا، کلسترول بالا و دیابت را کنترل کنید.
- رژیم غذایی سالم داشته باشید.
- بهطور منظم ورزش کنید.
- ورزشهایی از قبیل قدم زدن، دوچرخهسواری، برداشتن وزنههای سبک و حرکات کششی انجام دهید.
- هر روز این تمرینات را انجام دهید، اما زیاد خود را خسته نکنید و از انجام فعالیتهای شدید خودداری کنید.
- به اندازه کافی بخوابید.
- کمتر به خود استرس وارد کنید.
- نمک کمتری میل کنید؛ نمک باعث میشود سیالات در بدن شما ثابت باقی بمانند، که این به قلب شما آسیب میرساند.